Student Blog
Erika

USC’s Student Run Clinic: Providing Care to the Underserved in Skid Row ⟩
November 13, 2017, by Erika
One of my top 3 enriching experiences in this program didn’t take place in the classroom and wasn’t at fieldwork. It was in a men’s shelter located in the middle of Los Angeles’ Skid Row. It was here where I met Ben*, a man who was living at the shelter that came to see us at the Student Run Clinic because he was complaining about itchiness on the bottom of his feet.
Hold up, what is Student Run Clinic?
Student Run Clinic is a student run organization that provides comprehensive healthcare to the homeless, chronically ill, and underserved populations in Skid Row. We work in an interprofessional team alongside students from USC’s Medicine, Physician Assistant, and Pharmacy programs operating two clinics monthly — one at John Welles CH (JWCH), a Federally Qualified Health Center (FQHC) one Saturday morning a month as well as a mobile clinic that operates out of a men’s shelter on one Tuesday evening a month.
Gotcha, back to Ben.
Ben came to see us on a Tuesday evening in which we set up shop in the men’s shelter he was staying at. As part of the clinic protocol and as the OT student, I was the first to greet Ben and introduce him to what he was going to experience throughout the course of the night. I then gathered his social history — asking him questions about life before living in the shelter, how he occupies his time during the day, if he has plans for what’s next, who his support system is, what his current employment status or past employment history is, etc. We got to talking and because clinic was running a little slow, I had time to chat him up more than usual.
Ben was a biking barber. He spent his days making money cutting hair biking across Downtown Los Angeles and was proud of it. A couple weeks before I met him, he had traveled to a bike race in Northern California and during that time, his landlord rented out the apartment he was living in without telling him leaving him homeless when he came back to Los Angeles. Thus, his current situation of living in the shelter. Despite these setbacks, Ben was upbeat in demeanor — honoring the hustle, doing what he can do to work as much as he can, confident and capable. I really enjoyed meeting him. I asked all my curious questions about being a biking barber and he asked me about being a student. ::knock knock knock:: My time was up.
After I left the room, I briefly summarized what I learned to the team (2 med students, 1 pharm student, and 1 PA student). It was there turn now to go in and ask their questions specific to their specialties. Med and PA took Ben’s vitals and administered the physical exam on his feet. Pharmacy inquired about any current medications he was taking, whether he was satisfied with those medications, if the medications affect the itchiness on his foot, etc. :: knock knock knock:: Their time was up.
While Ben was speaking with the other students, I was busy consulting our faculty preceptor, Dr. Pitts about everything I learned about him to work through the case. She helped me clinically reason through the case and ensure we have all the information we need to inform the team on a potential treatment recommendation. At the time when I met Ben, Dr. Pitts proctored both clinics but now Dr. Erin McIntyre has taken over mobile clinic and Dr. Pitts focuses on Saturday clinics at JWCH. If there’s anything I can be grateful for in volunteering and serving on SRC board, it’s the unwavering guidance and experience of our faculty mentors.
Once all the other students returned from speaking with Ben, we engaged in “the Huddle” — the point in the night where we share all the information we learned about the patient and as a team, create a problems list and potential treatment plan accordingly. Once this was agreed upon, our attending physician, Dr. G, came in to hear us present all of our findings. As an educator and mentor, Dr. G provided us with feedback, constructive criticism on where we may have had some holes in our questioning or evidence, and a cohesive understanding of any next steps.
While Ben was a rather simple case of determining whether he had dry skin or a fungal infection, the experience was so much more than that.
- I was able to listen to Ben’s story firsthand and gain a tiny ounce of understanding of his experience living in Skid Row.
- I thought critically in an OT lens and assessed his living conditions, daily occupations, and motivation to inform us about his foot and skin condition and his ability to follow through on treatment.
- I was able to make new friends in other professions, delve into each others healthcare lens, and understand how each profession contributes to a primary care model.
- Lastly, I was able to advocate for Ben in providing the other health care professionals insight into Ben as a human outside of being a patient.
Being a part of Student Run Clinic has been a true privilege and one I would never pass up for anything in this program. It’s an experience that is unlike any other and if you’re currently a student in any of USC’s programs (Medicine, Physician Assistant, Pharmacy, or Occupational Therapy), I would encourage you to volunteer. You won’t regret it.
*All names mentioned in this blogpost are pseudonyms.
⋯

A Day in the Life of a USC Entry-Level Master’s Student ⟩
October 20, 2017, by Erika
Hi all!
Inspired by the Day in the Life of a Chan Student feature on the Division’s website, I thought I’d provide you with a breakdown of what a day may look like for me as a 2nd year Entry-Level Master’s student. My schedule is a little different everyday based on work hours as a student ambassador, my Level I fieldwork placement, and having Fridays off, but here is what a typical day may look like if I had a full day of classes. This is also similar to what a 1st years day would look like since they have the same 2 blocks of time carved out for classes.
A Day in the Life
7:20 — Alarm goes off! Snooze.
7:30 — Wake up! Get ready, make breakfast, pack lunch.
8:15 — Out the door!
8:35 — Look for parking around HSC.
Note: It’s LA! Parking will always be an issue. As a student, you do have the option of purchasing a parking pass on campus. If you choose to opt out of that option, you’ll have to do a bit of a morning hunt like I do to find free parking in the local neighborhood. I would say that after the first few weeks, you’ll get really good at figuring out the best places to park - not to mention know the street cleaning signs by heart! This option also allows for nice morning and afternoon walks to and from your car!
9:00-12:00 — Class
Note: Typically we will get (2) 15 minute breaks to stretch, reset, take a walk. During 1 of the breaks, you’ll probably see me at Eric Cohen Student Health Center getting free coffee, tea, or hot chocolate offered to all USC students!
12:00-1:00 — Lunch
Note: Many times, faculty, student orgs, or the health center may schedule meetings during lunch on various topics: Doctorate or PhD info sessions, Mentor/Mentee lunches, mindfulness classes, yoga on the lawn, etc. If I’m not at one of these, you may see me eating with friends on the patio or practicing transfers with them in the ADL lab.
1:00-4:00 — Class
Note: Afternoon classes can be tough so the free coffee break may happen at this point of the day. Good thing is, since our professors are OTs, they are very attuned to reading when the students are having attention difficulties or hitting an afternoon wall. They’ll break things up, encourage us to stand, take walks, or if we’re in the pediatrics classroom, swing on the swings for some self-regulation!
4:00 and on — Open!
Note: After class, what I do really varies depending on the day. I may have to work in the Student Ambassador office. I may have a meeting for Student Run Clinic. Perhaps I’ll hit up a yoga class, go to Barbara’s at the Brewery with a few friends for a beer, or visit my niece and nephew to play and have dinner! Either way, I find weekday afternoons as opportunities to decompress and chill after a full day of class.
11:30 — #sleepgoals
Thanks for reading! If you have any questions, feel free to write in the comments!
⋯

Standardized Patients: the Good, the Bad, and Becoming the Hulk ⟩
October 6, 2017, by Erika
One of the best opportunities our program offers is the chance to practice transfers with standardized patients in our Adult Rehab immersion.
What’s a standardized patient?
It’s a person carefully recruited and trained to take on the characteristics of a real patient providing students with the opportunity to learn skills in a simulated clinical environment. Neat, right?
So far in my adult rehab immersion, we’ve practiced with standardized patients “recovering from hip replacements, back injuries, and stroke.” We’ve learned how to transfer them from laying in bed to sitting then to a wheelchair or walker! From there, we’ve also practiced how to mobilize and transfer these patients to the shower, tub, and toilet.
It’s been ADLmania!!!
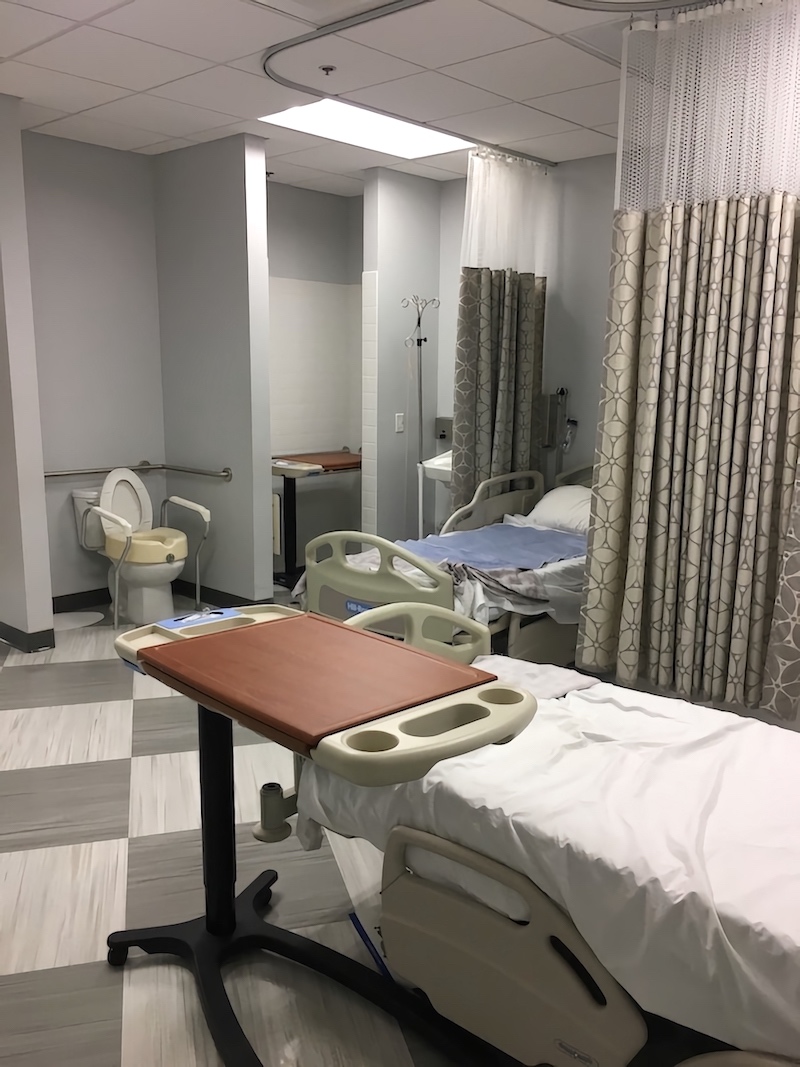
Our Adult Rehab lab was designed to simulate common practice locations where we would actually conduct transfers and treatment sessions. On one side, we have an exact replica of what a hospital room looks like at Keck Medical center — from the beds to the toilet and shower. On the other side, we have a standard bedroom with access to a tub and toilet. Lastly, we have a fully functioning kitchen where we can practice various occupations like meal prepping, washing dishes, and cooking. What’s better than practicing real life occupations in a real life setting?


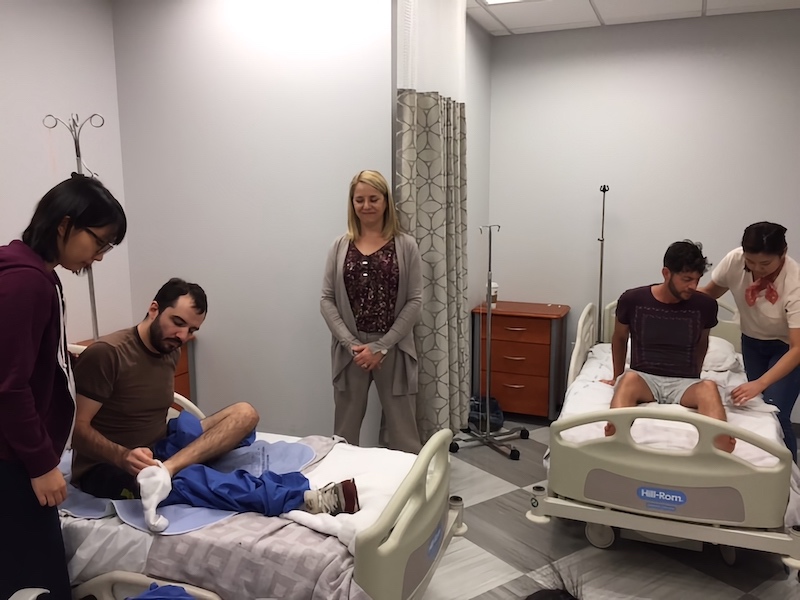
Readers, can I just say, the first time I practiced with standardized patients, I. Was. Terrified.
“I have NO clue what I’m doing. Are they going to be nice? Are they going to be painfully dramatic? Am I going to drop someone and break their hip a second time?”
My stream of consciousness spiraled into the dark depths of the unknown but of course, with all new experiences, it wasn’t as bad as I thought it was going to be.
Sure, I think all of us students will admit that the first time, there was a lot of “uhhhhh . . .”s, big perplexed eyes, and unnecessary overexplanations of the protocol running through our heads and out our mouths. After that though, you realize that the standardized patients aren’t there to give you a hard time or to give Oscar-worthy dramatic performances but are there for you and your learning experience. While at times, they were committed to simulating pain (which was intimidating at first), they were incredibly kind and open to providing feedback on why they felt pain or felt discomfort. They were gracious in giving us as many opportunities to try again to make sure we get a specific transfer or handling right.

At the end of the day, that’s what makes the opportunity of practicing with standardized patients valuable — it gives us the opportunity to spiral into our own fears then build ourselves back up with the support and feedback of our professors and standardized patients to reveal our own capabilities and strengths — all within a safe learning environment!
I want to close with some advice I was given while working with a standardized patient named Mel*. After I had transferred him, he looked me straight in the eye and said, “You have to commit. If you don’t commit, I won’t commit.” I’m not sure if this was a reflection of his practices as a method actor, but it completely changed how I transferred after that point. I became more confident. You know when Bruce Banner becomes the Hulk? It was like that without all the rage. Mel’s words transformed my identity from being a timid inexperienced OT student to a potentially strong, capable, and committed OT practitioner. Thanks Mel.
*All names mentioned in this blogpost are pseudonyms.
⋯

New to LA? No Worries! ⟩
September 19, 2017, by Erika
Every LA native has their list of go-tos to take people when they visit but they also have their smaller, more intimate list of what a friend of mine calls, “secret squirrel spots.” These are places that are just a little more special. For me, they are places that have grown my eyes a little bigger, made my heart a little softer, or tickled my tastebuds like never before. I hope that by sharing these with you all, you will find them as beautiful, meaningful, and as memorable as I have. Whether you’re new to LA or not, go, explore, and be merry!
SuihoEn Japanese Garden, Van Nuys
An oasis in the middle of the city! It’s one of my favorite hidden places in LA and it’s only $5 to enter. As you venture through the garden, you’ll find a tea house. I’d recommend bringing some hot tea in a thermos and a friend and have yourself a little tea party overlooking the koi pond.
El Matador State Beach, Malibu
Being in LA, you have an entire coast of beaches to choose from! After venturing from the valley to the OC, I still reserve a special place in my heart for El Matador State Beach up by Malibu. There are rock formations there that transfer you to another planet. Climb them, crawl through them and find little crabs, or find a little cave to take a nap in!
LASA, Chinatown
What’s LA without good eats and what’s an LA experience without supporting local chefs? I knew these two brothers, Chad and Chase, from high school and seeing them blow up on the LA food scene featuring food I grew up with brings tears to my eyes. Born and bred in aroma-filled Filipino homes, they’ll provide you with an innovative yet authentic taste of Filipino cuisine.
The Great Wall of LA Mural, North Hollywood
After hearing about it for years, I only visited this gem about a year ago and regret not visiting sooner. This was a community project done by more than 400 community youth, their families, artists, oral historians, ethnologists, and scholars depicting the history of Los Angeles from 20,000 B.C. all the way up to the 1960s. It’s a half-mile long and a great way to spend the afternoon learning about the city you’ve found yourself in! Be sure to pop this into your phone (sparcinla.org/the-great-wall-part-2) to guide you through your historical and visually stimulating experience.
If you end up visiting any of these spots, leave a comment and let me know how you liked them!
⋯

No OT to shadow? No worries! ⟩
September 6, 2017, by Erika
To those of you who are currently in or still need to complete the mental health immersion, this blog post is for you. Many of you have concerns about not having an OT to shadow during your level I due to the limited number of mental health facilities that have OTs available. That’s a fair concern, I had the same one! Fear not, I’m here to say that I had a great experience in my level I even without an OT to shadow. It took a bit of a perspective shift but once I was able to allow the experience to reveal itself naturally, what I ended up gaining exceeded any expectations and fears I had going in.
During my first fieldwork placement during my first year, I was placed at Verdugo Hills Hospital’s geriatric psychiatric unit called Stepping Stones. I had the opportunity to observe both inpatient and outpatient settings which was quite a privilege. As with most mental health settings, there was no OT to shadow. Therefore, I was placed under the supervision of two recreational therapists and an art therapist in the inpatient unit as well as two social workers in the outpatient unit.
Here is what made my mental health experience so valuable even without an OT to shadow:
- I learned what professions are already well established in mental health, what they do, and how OT can provide additional value. Before this fieldwork, I didn’t know much about mental health. I just assumed that if someone had mental health issues, they’d see a psychologist. Through this fieldwork, I had the opportunity to observe interventions done by recreational therapists, an art therapist, and social workers and how they played their parts in assisting patients across the progress of their illness. I learned that in art therapy, you would choose mediums (markers vs. paints vs. colored pencils) according to the patients’ cognitive levels and abilities as well as the psychological significance of certain colors! I learned that social workers have the authority to diagnose and observed how they engaged clients in group talk therapy. Best of all, I was able to execute OT sensory and cognitive interventions and inform the other professions on what value we could bring to what they were already doing. It was a beautiful exchange of thought across professions and a shared passion of service to this population.
- I was able to get exposed to all mental health settings through the experiences of my peers and in turn, reduce stigma that I personally associated with mental health. Since there are few OTs to shadow, mental health is the only immersion in which weekly fieldwork debriefs are set up with peers and a faculty member during class time. I think that most of my classmates would agree that this served as being one of the most helpful resources. We were placed with the same group all semester in which each member was placed in a different mental health setting so we got firsthand experiences of what each setting entailed. What a way to learn! It provided an open platform to not only share in each other’s concerns and successes but gave us a deeper lens into the mental health community. These debriefs equipped us with awareness and compassion, and in turn, helped debunk any stigmas that we initially came into the course with.
- USC faculty support is top notch. Even with the lack of OT in my settings, there was never a time that I didn’t feel supported by USC faculty. With such breadth of experience, you are bound to find a faculty member that has practiced in the setting you’ve been placed in (inpatient, outpatient, full service partnership, wellness center, clubhouse, etc.). I was able to reach out to faculty members and pick their brains about possible interventions to try out, success stories, horror stories, etc. just to feel a bit more comfortable in understanding OTs role in my specific setting. This experience opened doors to forming relationships with faculty who I now see as mentors that I feel comfortable reaching out to for guidance throughout school and my future career.
- Developing my therapeutic use of self. Even without an OT, this fieldwork placement was a great opportunity to observe the variance in how my supervisors, as therapists, utilized their own therapeutic uses of self. Everyone has their own gifts, ways of communicating, and backgrounds that contribute to how they practice and work with clients. It was fascinating to see how one recreational therapist Carl*, who I called the Zen master, would engage patients vs. another, Yuko*, who was bubbly and charismatic. They were so different and yet, their concern and care for every patient was expressed and equally well received. This made me really reflect on the fact that there is no one way to be a successful therapist. I began to observe my own therapeutic use of self and develop my own style of practice utilizing my own authentic experiences and gifts.
I know this post was a bit of a big boy but thank you for reading. Hopefully, I’ve been able to alleviate some fears or at least provide a change in perspective on what else you could look forward to during your level I mental health fieldwork placement. At the end of the day, with all your fears, questions, or concerns, know that there is faculty close by, peers going through the same thing, and new and interesting perspectives that lie untapped with your supervising mental health professionals that might provide more insight into your own value and practice with this population. Level I placements are meant solely as a means to observe so OPEN YOUR EYES — you may be surprised by what you end up learning.
*All names mentioned in this blogpost are pseudonyms.
⋯








Social
Facebook Instagram LinkedIn YouTube